Cervical Cancer Remains a Global Health Issue

The widespread adoption of the human papillomavirus (HPV) vaccines and cervical screening across Australia and other developed nations has resulted in a significant fall in cervical cancer rates in many countries over the last decade. Nonetheless, cervical cancer remains a critical health issue worldwide and in Low- and Middle-Income Countries (LMIC) in particular.
Cervical cancer is the fourth most common cancer in women, with more than half a million women diagnosed with the disease in 2018(1). In low- and middle-income countries (LMIC’s) cervical cancer is the second most common form of cancer among women. About 90 percent of deaths from cervical cancer occur in LMIC’s(1).
Of all cancer screening methods, cervical cancer screening has been shown to be the most effective(2). Why then does cervical cancer remain a major health issue?
Unequal Access to Cervical Cancer Screening
Developed nations have vaccination and cervical screening programs that are widespread or adopted at a national level (such as Australia). Effective cervical cancer screening requires robust clinical infrastructure, skilled human resources and quality assurances − most of which are unavailable in LMIC’s, where resources are limited. Hence, these countries have less access to cancer screening and treatment options, and the mortality rate for cervical cancer is higher.
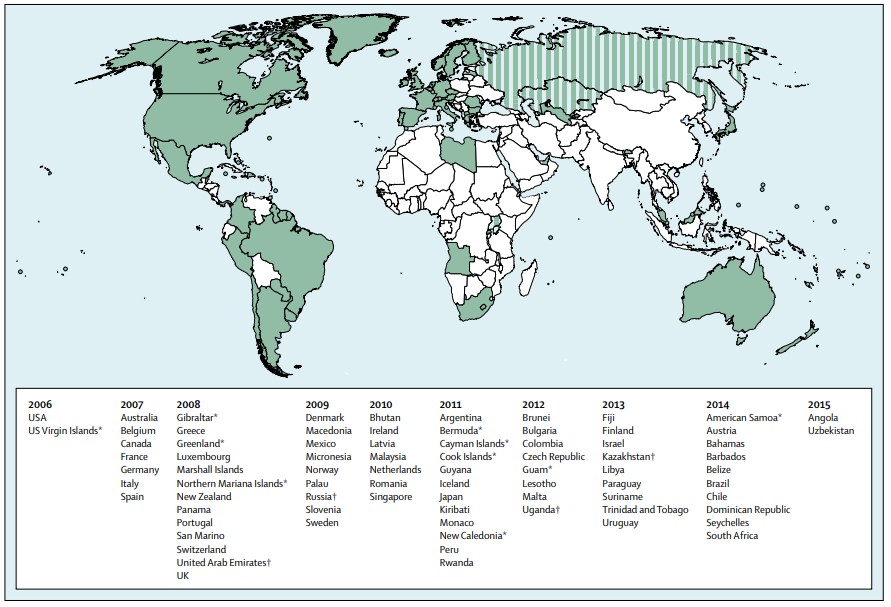
Additionally, nearly all cases of cervical cancer follow from infection by oncogenic HPV types (3). The development of screening opportunities using alternative HPV-based strategies and HPV vaccinations has greatly reduced the rate of cervical cancer. However, for LMIC’s, the implementation of HPV vaccinations is limited because of its high cost (see Figure 1 for a list of countries with publicly funding HPV vaccination programmes). Consequently, only 10 percent of females in LMIC’s have access to the HPV vaccine, compared to 90 percent of females in developed nations(4).
Publicly Funded HPV Vaccination Programmes Worldwide
Figure 1 (above): Countries that have introduced a publicly funded national HPV vaccination programme since 2006, by year. Striped sections indicate implementation in a part of the country.
Source: Bruni, L. Diaz, M. Barrionuevo-Rosas, L. Herrero, R. Bray, F. Bosch, F X. 2016. Global estimates of human papillomavirus vaccination coverage by region and income level: a pooled analysis. Volume 4, Issue 7, pages 453-463, https://www.thelancet.com/action/showPdf?pii=S2214-109X%2816%2930099-7
HIV and Cervical Cancer Among Women
Furthermore, there is a high correlation between women with HIV and cervical cancer. Cervical cancer is the most common cancer among women living with HIV(4). The likelihood that a woman living with HIV will develop invasive cervical cancer is up to five times higher than for a woman who does not have HIV4.
A large majority of deaths related to cervical cancer in LMICs occur in sub-Saharan African countries that have the highest burden of HIV4. For instance, in Zambia, the rate of cervical cancer is 10 times higher than in Australia. In Eastern and Southern Africa, women are 10 times more likely to die of cervical cancer than women in Western Europe(4).
Despite their increased risk of cervical cancer, women living with HIV in LMIC’s often do not receive regular screening or treatment for the disease. According to recent large studies, in Malawi and Zambia, only 19 percent and 27 percent of women aged 30-49 years who are living with HIV have been screened for cervical cancer(4).
According to the World Health Organisation, one of the fundamental steps to reducing the rate of cervical cancer worldwide is a comprehensive approach to cervical cancer prevention and controls1.
At TruScreen, we are providing a solution to the limited resources for cervical screening in LMIC’s through our breakthrough device that provides real-time reporting without the need for laboratory testing and which offers to women a more accessible screening option. The TruScreen device is primarily distributed in LMIC’s and offers an alternative approach to cervical screening, resolving many of the ongoing issues faced in these regions, including accessibility and the need for supporting laboratory infrastructure.
By improving access and supporting diagnostic screening and testing tools that help in the early detection and treatment of cervical cancer, we may be able to eliminate the disease worldwide.
References:
- World Health Organisation, Cervical Cancer, WHO International, 27 September 2019,https://www.who.int/cancer/prevention/diagnosis-screening/cervical-cancer/en/
- Hakama M, Miller AB, Day NE. Screening for Cancer of the Uterine Cervix.From the IARC Working Group on Cervical Cancer Screening and the UICC Project Group on the Evaluation of Screening Programmes for Cancer. WHO (Geneva), IARC (Lyon), and UICC (Geneva) 1986; 1–315 IARC Sci Publ. 76
- Arbyn, M. Castellsague, X. de Sanjose, S. Bruni, L. Saraiya, M. Bray, F & Ferlay, J. 2011.Annals of Oncology, Volume 22, Issue 12, December 2011, pages 2675–2686, https://doi.org/10.1093/annonc/mdr015
- UNAIDS, The little-known links between cervical cancer and HIV, UNAIDS, 27 September 2019, https://www.unaids.org/en/resources/presscentre/featurestories/2019/may/20190531_cervical-cancer-hiv